Vulvar Pain: everything you need to know
Vulva. Vagina. Vestibule.
So many V’s… and so much confusion.
And when you have pain down there…naturally we’re going to call it our vagina…but is it the vagina? Or is it the vulva? Or is it the vestibule?
If you’ve ever heard these words used interchangeably (or avoided altogether), you’re not alone. Clarity is empowering, and knowledge is one of the most important tools you have when it comes to pain, advocacy, and healing — so let’s break this down.
The Three V’s
Medical Terminology often pulls from Latin:
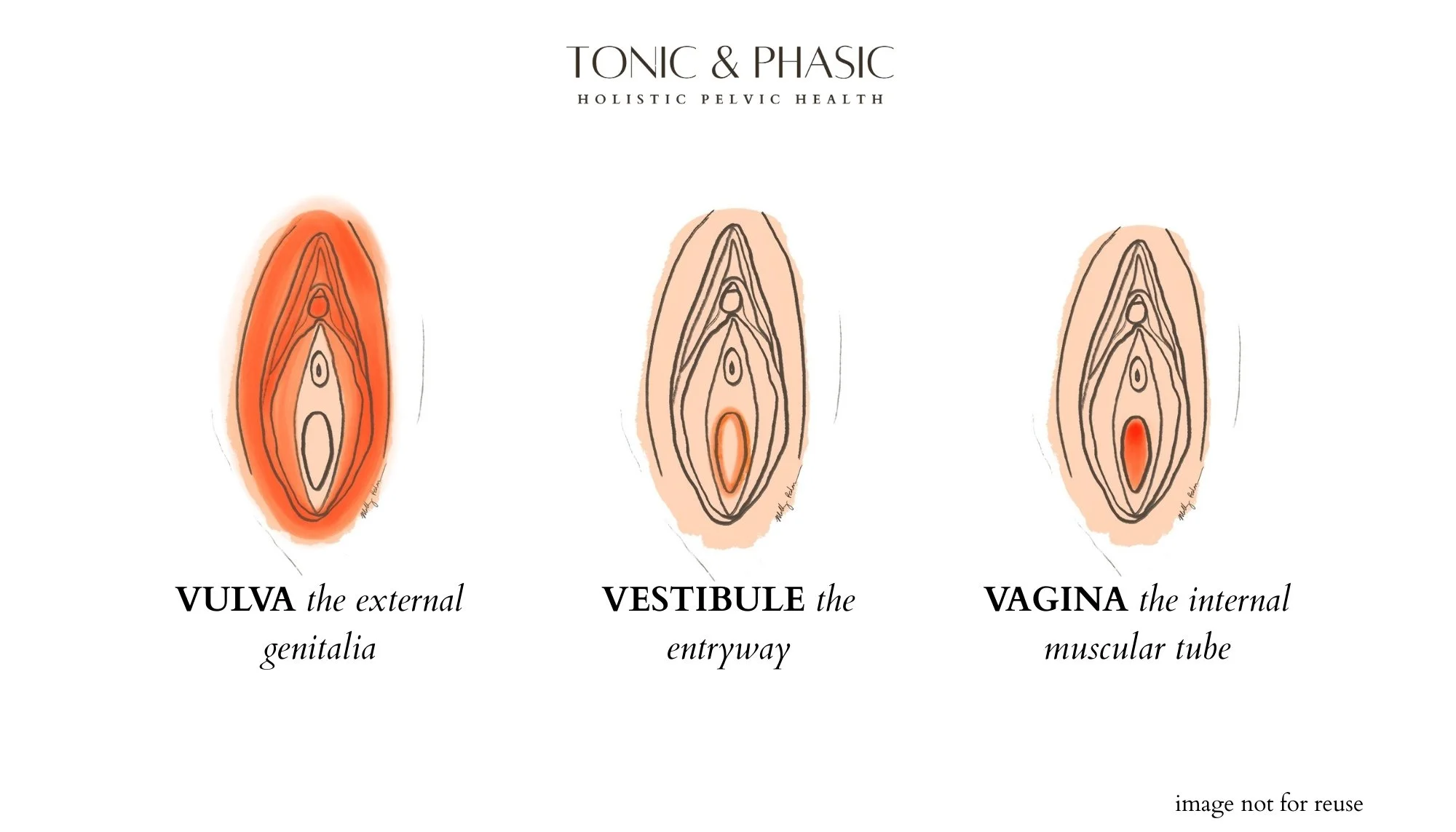
Vulva = the external genitalia. This includes the labia majora, labia minora, clitoris, and surrounding structures.
Vestibule = the entryway (also called the introitus). This is the space just inside the vulva that surrounds the vaginal opening and urethra.
Vagina = the internal muscular tube. The Vagina connects the vestibule to the cervix.
Every structure has different tissues, different nerves, and different implications for pain — therefore, treatment for pain in one of these areas will differ from treatment for pain in another.
When you experience pain or discomfort down there, you may wonder, “Am I the Only One?” The Short Answer is No.
Vulvar pain is common, even if it’s rarely normalized.
Research suggests that up to 1 in 6 people will experience vulvar pain at some point in their lifetime. Many experience symptoms for years before receiving a diagnosis, or are told everything “looks normal,” despite ongoing pain.
Our work is to change that narrative.
We’re here to help you understand your body better, put language to your symptoms, advocate for appropriate, comprehensive care, and know your treatment options.
So, how does pain in this area happen?
VULVODYNIA vs VESTIBULDYNIA
What is Vulvodynia?
Let’s break the word down:
Vulvo = vulva
Dynia = pain
Vulvodynia simply means pain at the vulva. Importantly, the emphasis is placed on where the pain is, not why it’s happening. This distinction matters because vulvodynia is not one single condition. It’s an umbrella term that can involve multiple contributing factors.
Regardless of the cause, vulvar pain may be:
Localized — specific spots
Generalized — widespread
Provoked — with touch, penetration, clothing
Unprovoked — present without contact
What is Vestibuldynia?
Vestibulodynia refers to pain that is specifically localized to the vestibule, the tissue surrounding the vaginal opening.
This area is richly supplied with nerve endings and is particularly sensitive to hormonal changes, inflammation, neural upregulation, irritation of the tissues, and even autoimmune conditions.
Pain in the vestibule is often described during:
Penetration
Tampon use
Gynecological exams
Prolonged sitting or tight clothing
THE PELVIC FLOOR CONNECTION
In vulvar pain conditions, the pelvic floor is very often involved, but not always as the original cause.
Pelvic floor pain specifically refers to pain driven by the muscles and connective tissues that support the pelvis. You may also hear us say “Pelvic Pain” which is a much broader term that can involve muscles, nerves, organs, joints, fascia, and the nervous system, which can all contribute to painful sensations in the pelvic region.
THE FEAR-TENSION-PAIN CYCLE
When pain persists, especially over time, the body adapts — sometimes in unhelpful ways. Pain leads to protective tension, particularly in the pelvic floor, abdominals, inner thighs, jaw, or glutes.
The muscular tension increases pain sensitivity and reduces circulation.
Fear of pain reinforces guarding and avoidance.
Over time, central sensitization can occur, meaning the nervous system becomes more reactive, even when tissue health has improved.
This is not “in your head.” It is a real, measurable nervous system response.
TONIC & PHASIC: HOLISTIC PELVIC HEALTH CARE IN ORANGE COUNTY, CA
causes, flare-ups, and treatment
CONTRIBUTING FACTORS TO VULVODYNIA
Vulvodynia can be present early in life (congenital) or developed later (acquired).
Holistic Pelvic Floor Therapy will look at common contributors with you, educating and empowering you along the course of your treatment. These contributors often include:
Hormonal factors like birth control, onset of puberty, postpartum, perimenopause, menopause
Autoimmune or inflammatory conditions
Muscular factors like pelvic floor overactivity
Dietary factors, including oxalate sensitivity, SIBO, yeast/candida contributors
Neurologic / neuroproliferative factors
Vascular contributors (e.g., pelvic congestion)
Psychological factors like trauma, or stress
WHAT MIGHT TRIGGER A FLARE-UP?
Many people notice vulvar pain flares with:
Certain medications (including estrogens or steroids)
Topical products
Fragrances or scented hygiene items
Tight or restrictive clothing
Prolonged sitting or pressure
Increased personal stress situations
Dehydration
Certain foods (acidic, spicy, high oxalates)
Intense exercise involving abdominal or lower body exercises
Vulvodynia is measurable, and it isn’t all in your head. So keeping your own journal of flare-ups can help you notice patterns and get curious about your body. Also, this journal can help your Pelvic Floor Therapist provide additional treatments to support you, so, win-win!
Treatment: A Multi-Modal Approach Matters
These conditions can be deeply distressing, but healing is possible.
Our strongest recommendation: Seek a holistic pelvic health therapist who is specialized in treating this kind of pain.
Our next tip: avoid doing everything at once.
Vulvar pain rarely exists in isolation. It often involves at least one or two of the below pieces:
Structural and physical imbalances
Hormonal influences
Nervous system factors
Inflammatory processes through various systems
Effective care looks at the whole picture and collaborates with you and other pelvic health experts to get the relief you deserve.
Pelvic Floor Therapy does far more than strengthen muscles. We also treat by considering the nervous system (the nerves involved in this region of the body are numerous), muscular and connective tissue health, movement and posture, breathing patterns, lifestyle and behavior contributions, and hormonal or inflammatory influences.
Pelvic Floor Therapy can help by:
Reducing tissue sensitivity and guarding
Interrupting the fear-tension-pain cycle
Providing pain science education (what’s happening and why)
Teaching safe movement strategies
Offering lifestyle and dietary guidance
Coordinating care with other specialists
Providing hands-on manual therapy when appropriate
Teaching stretches, breathing strategies, and nervous system regulation tools
Being another knowledgeable, supportive person in your corner
ADDITIONAL COMPONENTS OF CARE
Pelvic floor therapy
Sexual medicine physician
Gynecologist specializing in pelvic pain
Mental health or sex therapist
Nutrition and gut health support
A strong personal support system
Vulvar pain is common.
It is measurable.
And it is treatable.
Talking about it openly is not only validating, it’s often the first step toward meaningful change. Whether this is something you’re navigating now or simply learning about your body, knowledge gives you options, language, and agency.
And that matters.
Dr. Mallorie Hopkins and Dr. Allea Francis with Tonic & Phasic both specialize in Vulvodynia and would be happy to consult with you on a treatment plan. Book Now or explore our FAQs page for more information: