Understanding the Connection Between IBS, SIBO, and Pelvic Health
Irritable bowel syndrome (IBS) and small intestinal bacterial overgrowth (SIBO) are common digestive conditions that often overlap with pelvic symptoms.
Many who experience bloating, abdominal discomfort, or irregular bowel habits also notice pelvic floor tension, urinary urgency, or pelvic pain. Understanding the connection between the gut and the pelvis is a key step toward lasting relief.
To fully grasp how these conditions affect the body, it helps to consider the anatomy and physiology involved. IBS and SIBO primarily impact the small and large intestines, altering how food moves through the digestive tract and how gut bacteria grow. When motility slows or bacterial overgrowth occurs, gas, bloating, and discomfort can follow.
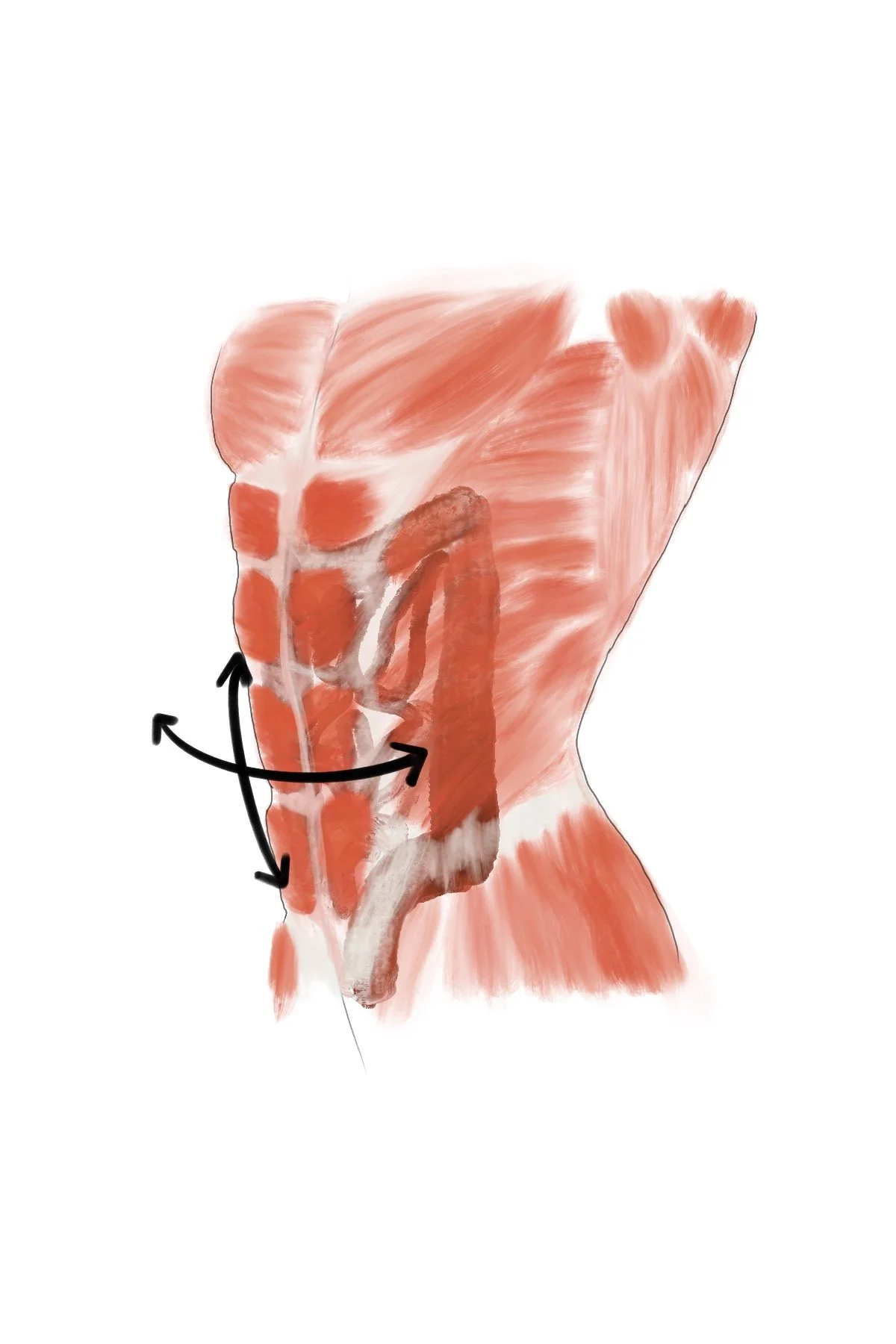
The abdominal wall
The abdominal wall acts as a supportive shield for your organs, helping maintain structure and stability. See the abdominal muscles protecting the intestines in the artists’ depiction. Chronic bloating or pressure can stretch and weaken these muscles, making the core less effective and leaving tissues more vulnerable.
artists’ depiction: not for reuse
The pelvic floor, a group of muscles at the base of the pelvis, supports the bladder, bowel, and reproductive organs. It works closely with the diaphragm and abdominal wall to coordinate pressure, movement, and elimination. When digestion is disrupted—through inflammation, tension, or irregular bowel habits—the pelvic floor can become tight, restricted, or poorly coordinated, which can worsen both digestive and pelvic symptoms.
Together, the gut, abdominal wall, and pelvic floor form an integrated system. Understanding how these parts interact is the first step in reducing discomfort and supporting both digestion and pelvic health.
At Tonic & Phasic, we take a holistic, full-body approach, addressing digestive health, core stability, and pelvic function together to create meaningful, lasting relief.
Why Bloating Matters
Bloating isn’t just uncomfortable—it can reveal a lot about how your gut and core are working. When your intestines get stretched from slow digestion, bacterial overgrowth, or inflammation, it can weaken your abdominal muscles. Over time, this makes your core less stable and tissues more vulnerable, which can lead to recurring bloating and digestive discomfort.
Your pelvic floor—the muscles supporting your bladder, bowel, and reproductive organs—works closely with your diaphragm and abdominal wall. When digestion is off, whether from inflammation, hormonal changes, or irregular bowel habits, these muscles can get tight or uncoordinated. That can make bloating worse and cause pelvic discomfort.
Looking Deeper: The Role of the Gut Microbiome
To find lasting relief, we need to look beyond diet alone. GI mapping is a tool we often use to understand your gut bacteria, inflammation levels, and overall microbiome health. This information helps guide personalized strategies for food, supplements, and lifestyle to support digestion and pelvic health.
Hormones and Digestion
Hormonal fluctuations play a big role in digestion and bloating. Prostaglandins, released during your period, can increase cramping, bloating, and digestive sensitivity. But estrogen, progesterone, and thyroid hormones also have a strong influence.
Estrogen: High estrogen levels can slow gut motility, leading to bloating and constipation. It can also affect fluid retention and inflammation, making abdominal discomfort worse.
Progesterone: Progesterone helps relax smooth muscle, including in the intestines. While this is important for overall function, elevated progesterone—such as in the second half of the menstrual cycle—can slow digestion and contribute to bloating and gas.
Thyroid Hormones: Thyroid imbalances, particularly hypothyroidism, can reduce gut motility, leading to constipation, bloating, and sluggish digestion. Proper thyroid function is critical for overall metabolism and smooth digestive rhythms.
Understanding how these hormones interact with your gut helps us time interventions and adjust strategies. Whether it’s targeted nutrition, lifestyle adjustments, or supporting hormone balance, addressing these factors can make a significant difference in reducing bloating, improving digestion, and supporting pelvic comfort.
Other Contributing Factors
Sometimes, other conditions can make bloating and pelvic discomfort worse:
Endometriosis: Can cause inflammation or adhesions that affect gut motility.
Scar tissue: From a C-section or abdominal surgery can limit internal organ movement, making digestion harder.
Structural or inflammatory conditions: Colonoscopies and other tests help rule these out.
A Holistic Approach to Support Gut and Pelvic Health
At Tonic & Phasic, we focus on a full-body approach.
Core & Pelvic Floor Work: Strengthening and retraining the core improves abdominal stability, posture, and coordination between the gut and pelvic floor.
Visceral Mobility & Scar Therapy: Gentle massage and targeted techniques help organs move freely, reducing discomfort.
Mindful Eating & Parasympathetic Support: Chewing thoroughly, breathwork, stress reduction, and routine help your body digest efficiently.
Gut Support: Prebiotics, probiotics, and nutrition strategies to promote a balanced microbiome.
Bringing It All Together
When the gut, core, and pelvic floor work together, the difference can be dramatic. An integrated, full-body approach can reduce bloating, improve digestion, and restore pelvic comfort. With a plan personalized to your microbiome, anatomy, and symptoms, your gut and pelvis can finally work together—supporting both health and overall well-being.
You can heal your gut. And a multi-provider approach including a pelvic floor therapist and holistic gastrointestinal provider can be hugely beneficial. Contact Us today to learn more!