Pudendal Neuralgia Explained: Why Pelvic Nerve Pain Happens (And What Helps)
Jordan remembers the exact moment things started to feel different.
Table of Contents
What is Pudendal Neuralgia?
What Pudendal Neuralgia Is (and what it isn’t)
Entrapment vs Irritation
What Happens Inside an Irritated Nerve?
How the Nervous System can Amplify Pain
What Quality Care Looks Like
It wasn’t a major injury. There was no dramatic event. Just a strange burning sensation upon sitting down at work one afternoon. At first Jordan thought maybe they had pulled a muscle or sat too long. But the feeling didn’t go away.
Over the next few weeks, sitting became harder. The burning turned into something sharper and more irritating—sometimes a shot of electric pain would zap right in the middle of the anus. Sometimes it felt like something stuck inside their rectum, despite just having gone to the bathroom. Other times it felt like heat or pressure near the sit bones.
Jordan started shifting in their seat constantly. Long car rides became miserable and made it worse. Sitting at dinner with friends suddenly felt impossible.
Eventually, Jordan began searching online. That’s when the fear started to roll in. Jordan read about “entrapped nerves”, permanent damage, surgeries, and conditions that were unheard of. And people had tried everything without hope. Some articles made it sound like once this nerve was irritated, life would never feel normal again.
But when Jordan finally saw a pelvic health therapist specializing in pelvic pain, the explanation was very different.
What Jordan was experiencing was pudendal neuralgia—an irritated pelvic nerve. And while the symptoms were real and understandably distressing, it didn’t mean Jordan’s body was broken. In fact, Jordan’s therapist responded to their anxiety with “Nerves are incredibly resilient and adaptable tissues. With the right environment and support, many people with pudendal neuralgia can calm the nerve, restore movement, and return to the things they love.” Immediately, relief set in, and things were going to get better.
If you’ve found this article because something in your body feels similar, you’re not alone—and there is more hope in this condition than many people realize.
Let’s start by understanding what this nerve is and why it can become irritated.
What Is Pudendal Neuralgia?
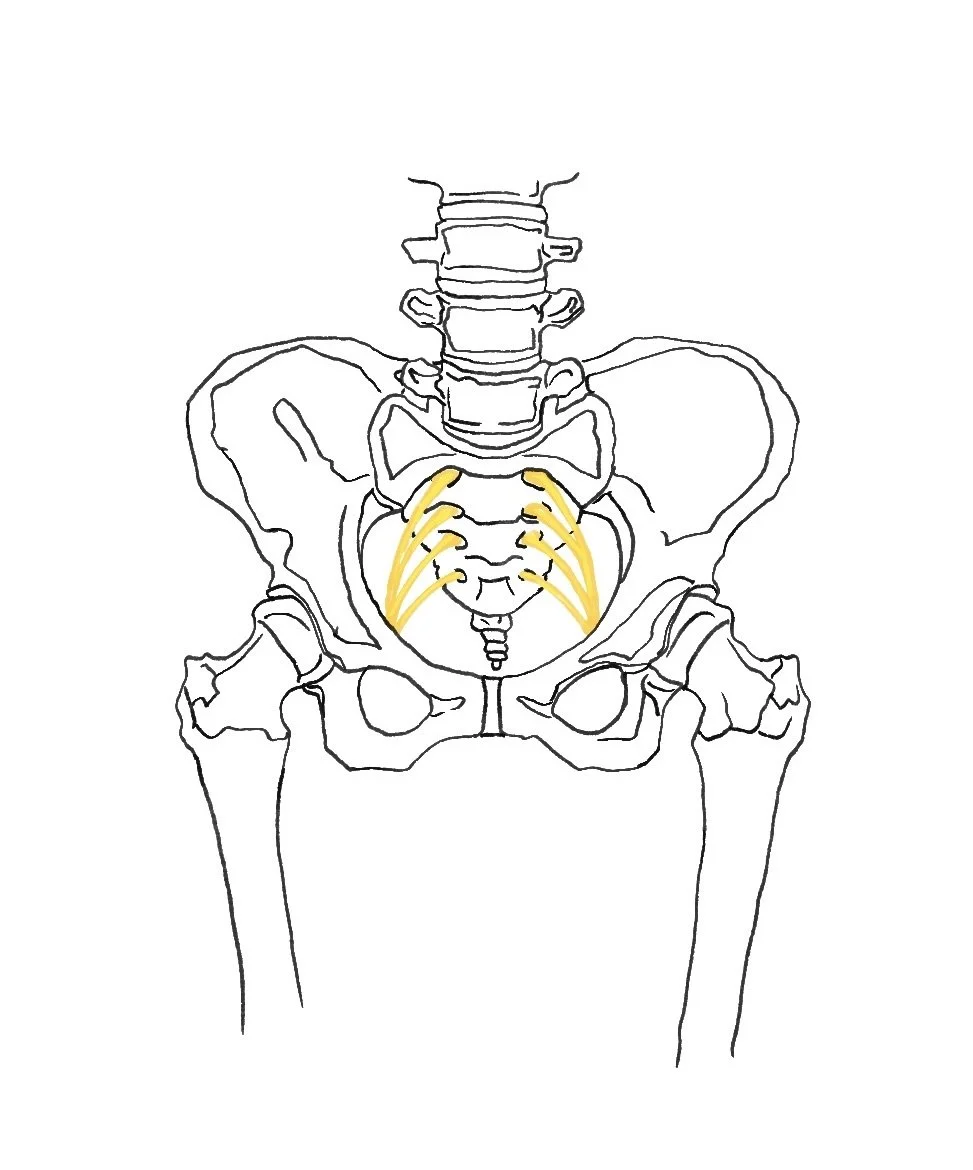
Pudendal neuralgia is a condition involving irritation of the pudendal nerve, one of the primary nerves of the pelvis.
As shown in the drawing (left), this nerve originates from the sacrum (S2–S4) and travels through the pelvis to provide sensation and motor control to several areas, including:
the external genitalia
the perineum (the space between the genitals and anus)
the end of the urethra
the end of the rectum
the external anal sphincter
portions of the pelvic floor
Because of where this nerve travels, symptoms often appear in areas such as the perineum, sit bones, anus, clitoris, or tip of the penis.
People with pudendal neuralgia often describe sensations such as:
burning or stabbing pain
electric or shock-like sensations
tingling or numbness
a feeling like something is stuck in the vagina or rectum
urinary urgency or frequency
pain during bowel movements with quick relief afterward
pain during or after clitoral orgasm or ejaculation
One of the most recognizable patterns of pudendal nerve irritation is positional pain. Many people notice that symptoms feel worse when sitting and better when standing or lying down. Interestingly, intercourse does not always worsen symptoms: clinically, this can be a clue that the pudendal nerve may be involved.
What Pudendal Neuralgia Is (and What It Isn’t)
When people start researching pudendal neuralgia, they often encounter explanations that feel incredibly scary. Many people are told their nerve is “trapped,” “permanently damaged,” or “something they will have to live with forever.” While pudendal neuralgia can absolutely be painful and life-altering, those explanations don’t always reflect the full picture.
Pudendal neuralgia is best understood as a spectrum of nerve irritation — and nerves are living tissues that can change, adapt, and heal when the environment supports recovery. Another important thing to understand is that this condition does not always show up on imaging. MRIs can help rule out structural concerns, but “normal” imaging results do not mean the nerve isn’t irritated.
Clinicians sometimes also evaluate for structural contributors such as:
Tarlov cysts
Annular tears in the spine
Lumbar nerve root irritation
Diagnosis of pudendal neuralgia often relies on patterns of symptoms and clinical examination, rather than a single definitive test. There is also a tool clinicians may use called the Nantes Criteria, which includes:
pain in the pudendal nerve distribution
pain worsened by sitting
pain that does not wake the patient at night
no objective sensory loss on exam
pain relieved with a diagnostic pudendal nerve block
In reality, not every case fits these criteria perfectly. Nerve blocks do not always provide clear answers, and nerves can be irritated at multiple points along their pathway.
Following this criteria is helpful in some cases, but in our clinical practice you don’t need to meet all five criteria for a diagnosis of Pudendal Neuralgia.
Another important point is that symptoms do not always progress gradually throughout the day. Some people notice pain building with sitting, while others feel symptoms immediately when they begin loading their pelvis in the morning.
Every nervous system responds a little differently. And that is an important piece of the puzzle: everyone’s story and healing journey is different.
Entrapment vs Irritation: Understanding the Difference
One of the most confusing parts of pudendal neuralgia is the word “entrapment.” Many people hear this and immediately assume the nerve is permanently stuck or damaged. But true pudendal nerve entrapment is actually less common than pudendal nerve irritation.
“Entrapment” means the nerve is physically compressed in a specific location, often due to structural changes or scar tissue. This can sometimes occur after:
pelvic surgery or procedures
deep suturing after childbirth
endometriosis or endometriosis excision surgery
scar adhesions near the sacrospinous ligament
egg retrieval procedures or IVF
When entrapment occurs, symptoms are often more mechanically predictable because the nerve is compressed at a particular site. However, many people diagnosed with pudendal neuralgia are actually experiencing nerve irritation rather than true entrapment.
In cases of nerve irritation, the nerve is sensitive due to factors such as pressure, stretch, inflammation, or surrounding muscle tension. Think of it like a bruise: the nerve becomes reactive and protective, but it still has the ability to calm down.
Regardless of whether the nerve is entrapped or irritated, pudendal neuralgia can improve. The treatment strategies may look slightly different depending on the presentation, but neither diagnosis automatically means permanent damage.
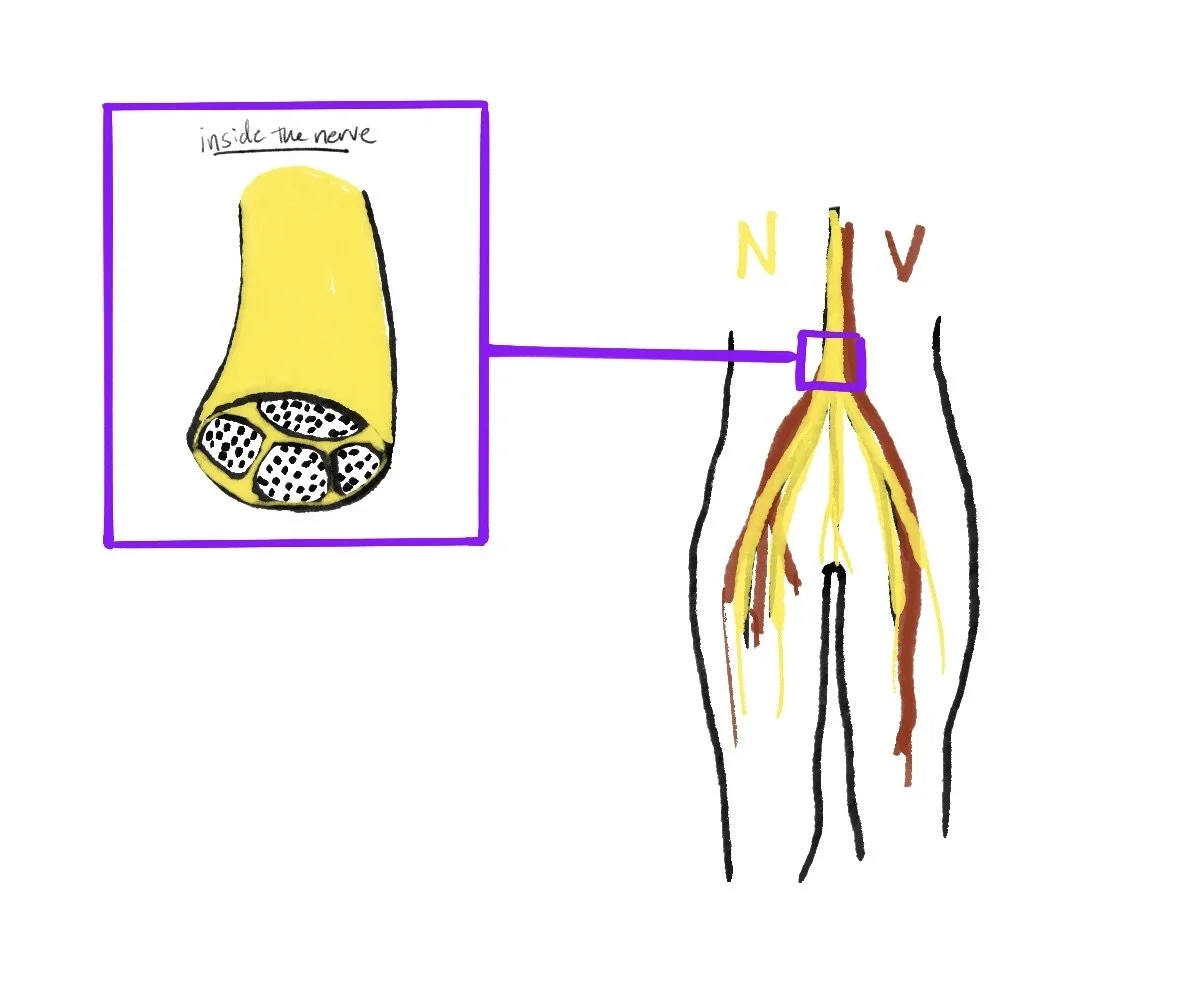
What Happens Inside an Irritated Nerve?
Our Nervous System (yellow) sits right next to our vascular system (red).
Inside each nerve are bundles called fascicles, which contain the small fibers responsible for sending signals through the body.
One of the most helpful ways to understand pudendal neuralgia is through a mechanical analogy.
Nerves are delicate structures; they do not like to be overstretched or compressed. When a nerve experiences too much pressure or stretch, it becomes irritated. But what happens next is fascinating.
Our nervous system sits right next to our vascular system, which includes arteries, veins, and lymphatic vessels. These systems deliver oxygen, nutrients, and immune support that help tissues heal.
Inside each nerve are bundles called fascicles, which contain the fibers responsible for sending signals through the body. When the outer nerve becomes irritated, the fascicles activate inflammation to protect themselves.
A helpful way to picture this is to imagine a car accident. The outside of the car may be damaged—but what matters most are the people inside. So the car deploys airbags. Airbags can sometimes cause small injuries themselves, but their purpose is protection: they prevent something much worse from happening.
Nerves behave in a similar way. When the outer nerve experiences compression or stretch, the inner nerve structures activate a protective inflammatory response. This response helps protect the nerve—but it also makes the nerve very sensitive for a period of time. Because of this, aggressive treatments or deep tissue work can sometimes make symptoms worse instead of better. Instead, healing often involves creating the right environment for the nerve to calm down—reducing pressure, improving circulation, supporting lymphatic drainage, and gradually restoring movement.
Sometimes in nerve care, less is more.
“Sometimes in nerve care, less is more.”
How the Nervous System Can Amplify Pain
If nerve irritation continues long enough, the nervous system itself can become more sensitive,andthe brain and spinal cord become more reactive to pain signals.This process is known as central sensitization.
People may experience:
pain that feels larger than what is happening in the tissues
widespread pelvic discomfort
hyperawareness of pelvic sensations
increased nervous system reactivity
Stress does not cause pudendal neuralgia, but it can amplify nerve sensitivity, which is why supporting the nervous system as a whole is often part of treatment.
Healing Takes Time
One of the most important things to understand about nerve injuries is that they heal slowly. During this healing process your body is becoming resilient, so this type of injury doesn’t happen again, and this process can take time.
For many people, healing and recovery happens over 6 to 18 months. That timeline can feel intimidating, but it also provides something important—a realistic roadmap for healing.
Nerves need time and the right environment to recover.
What Quality Treatment Looks Like
Treatment for pudendal neuralgia typically focuses on calming the irritated nerve and restoring healthy movement patterns.
Early care often includes:
Anatomy education and pain science education
Pain reprocessing therapy
reducing sitting pressure
pelvic floor relaxation
breathing and nervous system regulation
lifestyle support such as sleep and stress management
Developing new coping strategies
Some people benefit from tools like a RoHo cushion, which helps reduce pressure on the nerve while sitting.
As symptoms improve, treatment progresses toward restoring movement and strength. This may involve improving hip stability, supporting natural nerve mobility, and gradually rebuilding tolerance to sitting and daily activities. Progress is often measured not just by pain scores, but by returning to meaningful parts of life, like:
sitting at dinner with family
traveling comfortably
exercising again
reconnecting with intimacy
A Message of Hope
Healing from Pudendal Neuralgia in Orange County, CA
Many with pudendal neuralgia often feel like their world has suddenly become very small.
But many patients eventually find their way back to activities they once thought were impossible again.
Jordan—the patient we talked about earlier—did too.
Jordan’s progress didn’t happen overnight. It took patience, the right support, and a treatment plan focused on calming their nervous system and restoring movement gradually.
But eventually Jordan could sit at dinner, travel, exercise again.
And most importantly, Jordan no longer felt like their life was defined by pelvic pain.
Pudendal neuralgia can be incredibly challenging—but it is not hopeless.
Nerves are sensitive structures, but they are also capable of healing when the environment supports recovery.
One message we often tell patients is this:
Our bodies are resilient. Sometimes they become sensitive, but they are still capable of healing, adapting, and doing difficult things.
And with the right guidance and patience, healing is possible.