Bladder Pain Without a UTI: What Could Be Going On?
Frequent urination.
Urgency to urinate.
Burning with urination.
Pressure over the bladder.
Feeling like you need to pee but nothing comes out.
Or feeling like you never completely empty.
You go to urgent care, convinced you have a UTI… but your culture comes back negative. You follow up with a urogynecologist and everything looks normal.
So what’s going on?
This is one of the most common and confusing experiences we see in pelvic health. Many patients are told “everything looks normal,” yet their symptoms are very real.
When bladder symptoms are unexplained, the missing piece is often the pelvic floor. Tonic & Phasic Holistic Pelvic Health takes a comprehensive approach to determine why your bladder is irritated and how to treat the root cause.
Let’s walk through some of the most common reasons bladder symptoms can occur without an infection.
Bladder Anatomy & Physiology
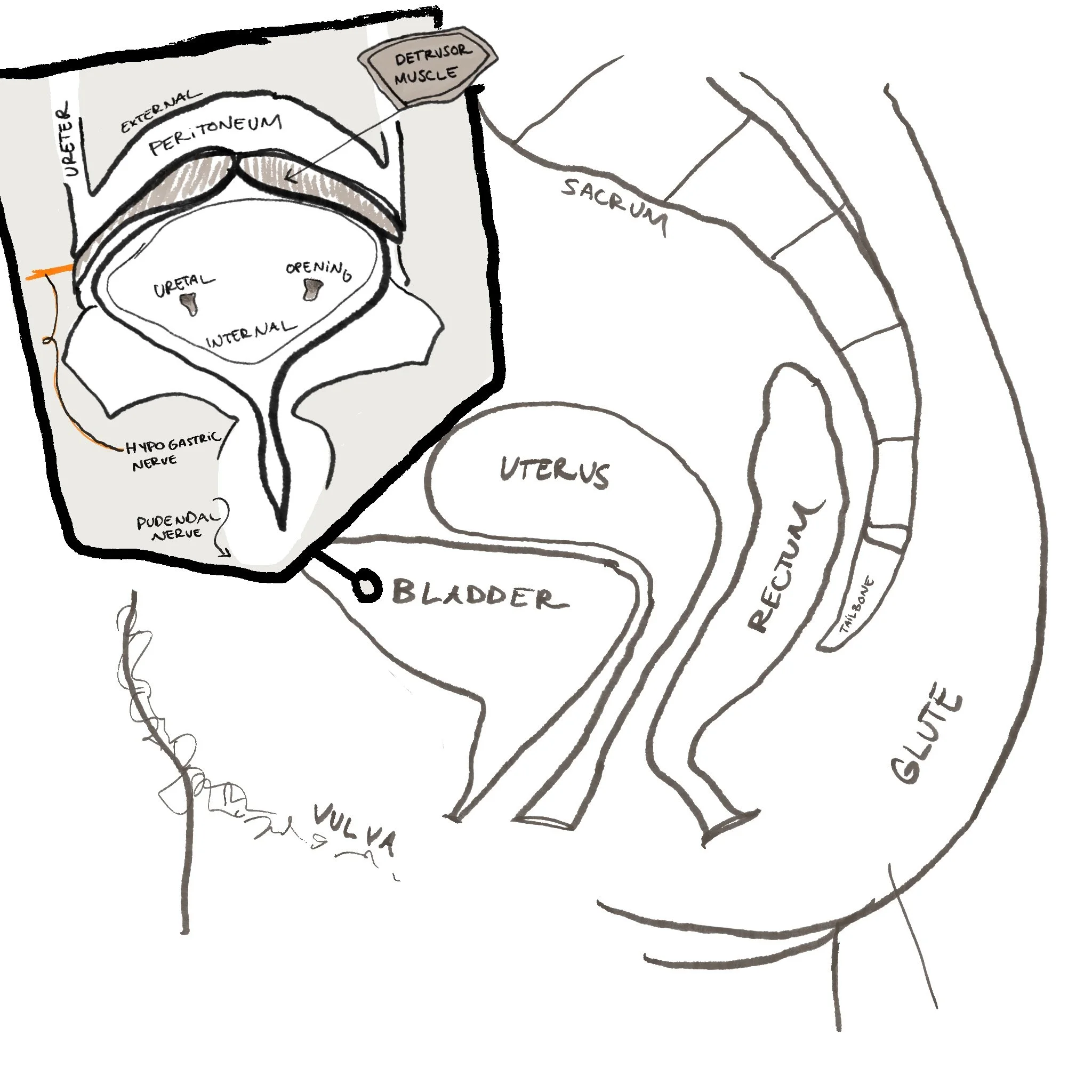
The bladder is a fascinating structure. It is supported by ligaments, surrounded by muscles, and deeply connected to our nervous system. Its main job is to store urine until it reaches about 400–600 ml, which is roughly 1.5 – 2.5 cups of fluid, about the size of a soda can to a small water bottle.
artist’s depiction
When the bladder is ready to empty, a muscle inside the bladder called the detrusor muscle contracts. As urine exits through the urethra, the internal and external urethral sphincters relax along with the pelvic floor muscles.
This process is controlled by both the autonomic nervous system and the somatic nervous system.
The sympathetic nervous system, our “fight or flight” system, communicates with the bladder through the hypogastric nerve, helping the bladder relax so it can store urine. The parasympathetic nervous system, our “rest and digest” system, communicates through the pelvic nerves, triggering the bladder to contract when it’s time to urinate. Lastly, the pudendal nerve gives us voluntary control over the external urethral sphincter.
As the bladder fills, stretch receptors in the bladder wall send signals to the brain. Most people receive two cues during this process. The first occurs when the bladder is about 40% full, which creates a mild awareness, making you think “I might need to go soon.” The second occurs around 80% full, when you begin actively thinking about finding a bathroom.
This second urge should not feel panicked or urgent. It should simply be a clear signal that it’s time to go.
Most people urinate every 2–4 hours, around 4–8 times per day, and each stream typically lasts 8–12 seconds. Fun fact: movies were historically designed to be under two hours long so people could watch the entire film without needing a bathroom break.
Understanding these patterns helps us determine when something in the system has been disrupted.
False Urges and Retraining
When bladder symptoms occur without an infection, we often describe the bladder as the “innocent victim.” Something else in the system may be irritating the bladder or disrupting its signaling. One common issue is what we call brain–bladder miscommunication.
If you urinate every time you feel the first signal, the bladder never fully fills. Over time, this trains the bladder to send signals earlier and earlier, creating a false urge. This can lead to a sensation that you constantly need to go, even when the bladder isn’t full — because the bladder has been trained to respond to smaller amounts of urine.
If you go to the bathroom and only urinate for 2–4 seconds or just produce a small dribble, you may be responding to these false urges.
This is where bladder retraining becomes important.
Often we begin with a bladder diary and then incorporate strategies to help suppress early urges and retrain the bladder to tolerate normal filling again. Let’s talk about one of these strategies: the freeze and squeeze.
When you feel that first urge to urinate, pause — don’t rush to the bathroom.
First, freeze what you are doing and acknowledge the urge.
Take a slow inhale and gently contract your pelvic floor (a light Kegel). This contraction sends a signal to the brain that the pelvic floor is closed, which tells the bladder to relax rather than contract. Do this 5 times with deep breathing.
Next, perform 10 calf raises. The bladder and calf muscles share similar nerve root levels in the spine, and activating the calves can help redirect the nervous system’s signaling away from the bladder.
After the calf raises, repeat the breathing and pelvic floor contraction again. Then try to distract your mind by continuing the task you were doing or by taking slow, relaxed breaths for about five minutes.
After five minutes, reassess.
If you still feel the urge, go ahead and use the bathroom, but pay attention to how long your stream lasts. If the urge has faded, continue waiting until that second signal appears.
The short-term goal is to reach one hour between bathroom visits, eventually progressing to two hours or more.
Another area we evaluate is the pudendal nerve, which plays a major role in pelvic floor and urethral control. If this nerve becomes irritated, it can send abnormal signals to the bladder and urethra, sometimes triggering spasms or sensations that mimic a urinary infection.
We also look at the nervous system as a whole. If the body is stuck in a chronic sympathetic (“fight or flight”) state, bladder sensations can become amplified. The bladder becomes more sensitive to signals, making urgency and pressure feel stronger.
Any disruption in this signaling system can influence how the bladder behaves. When urine cultures come back negative but symptoms persist, it’s helpful to look at how your bladder is functioning rather than assuming infection.
Start by keeping a bladder journal (download here) to track patterns in urgency and frequency, and try urge suppression techniques to retrain bladder signaling. If symptoms continue, a pelvic floor physical therapy assessment can evaluate the pelvic floor muscles and nerves to determine whether irritation or dysfunction may be contributing to your bladder symptoms.
The Bladder, Pelvic Floor & Pelvis
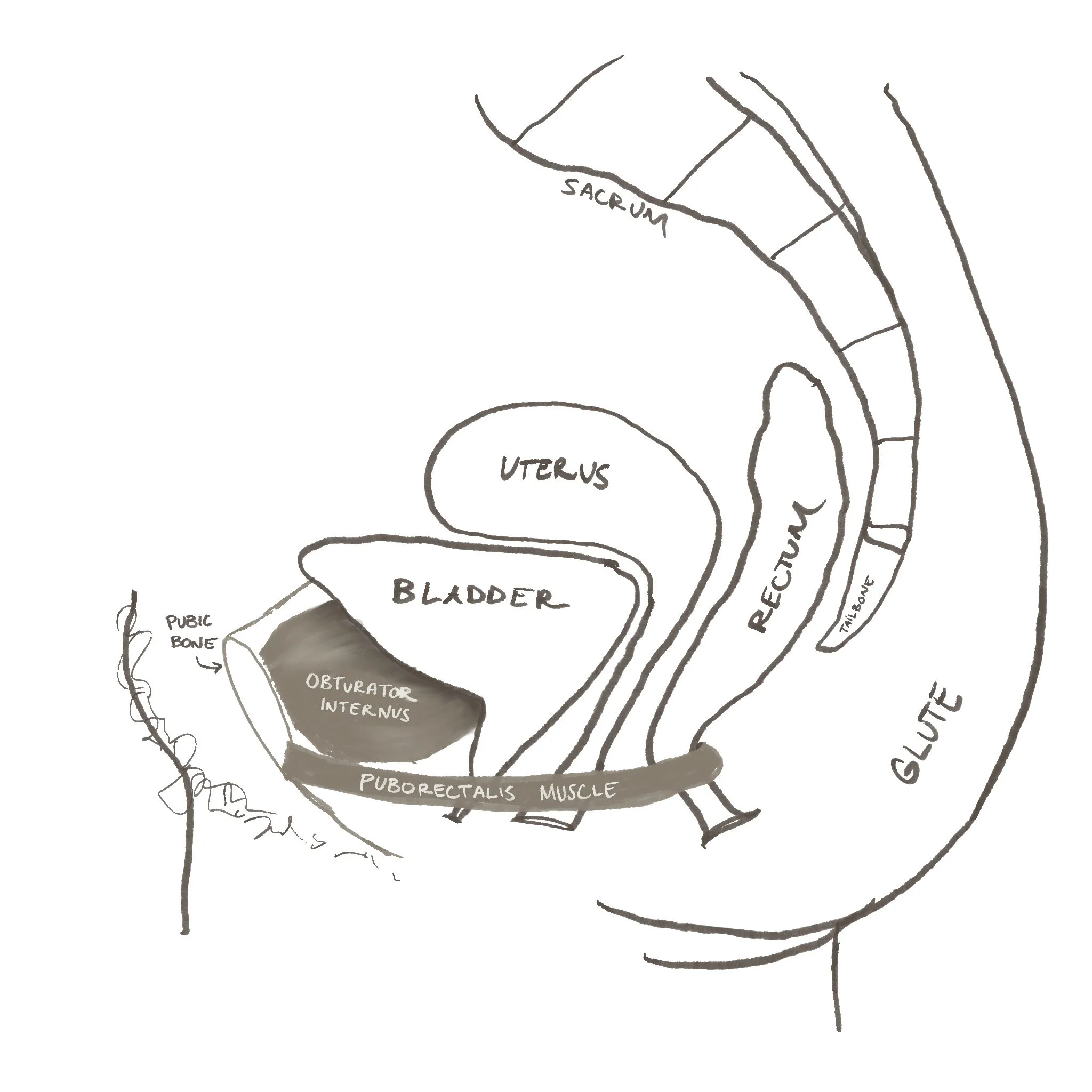
The pelvic floor sits at the base of the pelvis like a hammock, supporting the pelvic organs.
In order from front to back:
The bladder sits behind the pubic bone
The uterus sits behind the bladder
The rectum sits behind both
Because these structures sit so closely together, the way our pelvis is positioned or muscle tension can influence bladder symptoms.
For example, a posterior pelvic tilt can compress the front of the pelvis and reduce the space available for the bladder. This can create pressure sensations that mimic a UTI.
The tailbone is another important structure. If the tailbone is flexed forward, it can place pressure on the rectum, vaginal canal, and bladder. Since the bladder responds to pressure signals, this can trigger the sensation that you need to urinate or can contribute to incomplete emptying of the bladder.
Several pelvic floor muscles can also contribute to bladder symptoms.
The puborectalis muscle, which wraps around the rectum, sits close to the urethra. If this muscle becomes tight, it can irritate the urethra and create burning sensations or pressure near the bladder.
Another muscle called the obturator internus lines the side walls of the pelvis. When this muscle becomes tight, it can compress the bladder from the sides and send pressure signals into the lower abdomen, creating the feeling that you constantly need to pee.
If urge suppression strategies don’t resolve your symptoms, the next step is to look at these mechanical factors, or body factors, that may be contributing to bladder irritation. This is where body work and exercises are great to reduce your bladder discomfort.
The Bladder & Constipation
Constipation is a very common contributor to bladder symptoms. When the rectum fills with stool, it naturally creates pressure, which signals the anal sphincter to open and allow a bowel movement. This mechanism is meant to relieve pressure daily, but when bowel movements aren’t regular, the pelvic bowl can experience prolonged pressure.
Constipation can result from tight pelvic floor muscles, a forward-positioned tailbone, or a puborectalis muscle that doesn’t relax properly—leading to stool that may not fully empty. When stool accumulates, it presses directly against the bladder, creating lower abdominal discomfort, urgency, and frequent urination.
If constipation is contributing to your bladder symptoms, addressing gut health can be a key step in improving bladder function. Check out our Root Healing the Gutblog to learn strategies for relieving constipation and see if it’s playing a role in your bladder discomfort.
The Bladder & Hormones
Hormones also play a significant role in bladder health.
Estrogen and testosterone help support the tissues of the urethra, while estrogen also helps maintain the bladder lining. When these hormones decrease, the tissue can become thinner and more sensitive, leading to burning sensations, urgency, and frequent urination.
This is especially common during menopause, which is why hormone therapy can sometimes significantly improve bladder symptoms.
For individuals who are still menstruating, hormone fluctuations may still play a role. Supporting hormonal balance can often help regulate bladder irritation as well.
At Tonic & Phasic, we also offer hormone coaching, helping patients explore whether their cycle or hormone balance may be contributing to their symptoms.
Sex, the Bladder, and Post-Intercourse Care
Do you often experience bladder or pelvic pain after intercourse? This is actually one of the most common issues we see, and it can be triggered by a variety of factors—tight pelvic floor muscles, pelvic positioning, and other factors we’ve discussed in earlier blogposts. But there is also an interesting behavioral pattern we often notice: frequent urination after intercourse.
Most the time once we are finished we are told to use the bathroom to prevent a UTI. And here’s a key point: frequent urination can reinforce a feedback loop that keeps bladder urgency high. For example, if you urinate just before intercourse, the bladder usually takes 2–4 hours to refill. Urinating again immediately after intercourse can actually irritate the bladder and mimic a UTI. Confusing, right?
Let’s talk about post-intercourse care. If semen is inside, it’s important to sit on the toilet to clear it out — this is because semen can actually alter vaginal pH. If your pH is already more alkaline, this can cause general vaginal irritation, which may create pelvic tension and bladder discomfort.
For individuals who experience negative UTI cultures but still feel irritation after sex, we sometimes recommend skipping the immediate post-sex urination and instead cleaning the vulva thoroughly with a wash cloth (or toilet paper) with water or showering. This helps maintain hygiene without unnecessarily irritating the bladder. Important note: if you are experiencing confirmed UTIs with positive cultures, this recommendation is not for you.
If you find yourself rushing to the bathroom right after intercourse, try taking a moment to let your heart rate settle. Calmly walk to the bathroom and clean yourself thoroughly without immediately urinating, and see if this helps reduce the intensity of your symptoms.
Taking a Deeper Look
If symptoms continue despite pelvic floor therapy and behavioral changes, we take a deeper investigative approach.
This may include screening for mast cell activation or histamine intolerance, which can irritate the bladder. We may also evaluate oxalate intake, which can contribute to bladder sensitivity in some individuals.
Additional referral for medical testing may involve a cystoscopy to evaluate for interstitial cystitis with Hunner’s lesions. We may also refer to an endometriosis excision specialist, since endometriosis lesions can sometimes develop on the bladder and mimic UTI symptoms.
Other testing options include vaginal microbiome testing to screen for ureaplasma, mycoplasma, or biofilms, as well as deeper gut health testing such as a GI Map.
The most important thing to remember is that if symptoms persist, we keep looking. This is where we gather our team and start referring you to get more answers.
Summary
Bladder pain when your tests keep coming back negative can feel incredibly frustrating. Many people begin to feel dismissed when they repeatedly hear that “everything looks normal.”
But the truth is that bladder symptoms are often connected to multiple systems in the body, including the pelvic floor, nervous system, digestion, and hormones.
If you’ve been struggling with bladder pain, urgency, or frequent urination without clear answers, there may be more to the story than just UTIs.
At Tonic & Phasic, we take a whole-body approach to uncovering the root cause and helping you finally find relief. We look forward to supporting you.